
Excuse me, I took an unintended break for Thanksgiving! Hope you all had a wonderful holiday!
NaBloPoMo 2017: Field Notes from a Life in Medicine
For the past year or so, maybe more, I have increasingly tried to engage my friends in discussion around allied advocacy for physician health and well-being. Inevitably, however, I’m met with anecdotes from my friends about asshole doctors. It is a strikingly common experience, I’m sad to report. And it makes sense: If a patient has a bad experience with a doctor, ie the doctor behaves badly or the patient feels dismissed, ignored, disrespected, or mistreated, the normal response is to blame the doctor and assume that s/he is an asshole. In each of these interviews with friends, it took a while for them to come around to the idea that the doctor him/herself may be suffering and therefore not behaving/performing their best.
But the next question is this: Do patients care about doctors’ suffering? If they knew how the system harms physicians, would they have compassion for us? What about if they knew how physician burnout and dissatisfaction directly affects their quality of care, all of it negatively? What would move patients to stand up with and for doctors? This is my goal for the indefinite future: to help us, patients and physicians, the end users of our medical system, stand up with and for one another, for positive systems change.
Right now I see it as a very personal, grassroots endeavor. Outside of a one-on-one patient-physician relationship, ‘patients’ and ‘physicians’ in general are abstract groups to us all, and it’s hard to feel compassion for and connection with an abstraction. “Patients are too demanding, entitled, and ignorant.” “Doctors are arrogant, dismissive, and profit-driven.” We carry these overgeneralized internal narratives and others into our encounters, often unknowingly and unintentionally. Even when we think we see and know the person right in front of us, these underlying assumptions still color our experiences with them. So whatever conversations we may undertake will take many repetitions to finally reach true mutual understanding.
I have been a member of my church since 1991. Many others in the community have been there much longer than that. There are other physicians, and we are all patients, ranging in age from infants to octogenarians. I have proposed to host a focus group to discuss patient-physician relationship, especially as it relates to the effects of physician burnout on patient care. The plan is to do it once, with whomever is interested, and see what happens after that. I picture 10-20 people, patients and physicians alike, seated in a circle.
The objectives will be stated:
- Hold an open discussion about people’s experiences in the patient-physician encounter, and explore the context of forces that influence those experiences. Such forces include visit duration, documentation requirements, workflow inefficiencies, patient expectations, insurance status, and clinical setting (hospital, outpatient clinic, etc.).
- Participants leave with improved mutual understanding of one another’s experiences in the medical system and more likely to feel empathy and compassion toward their counterparts in the next encounter.
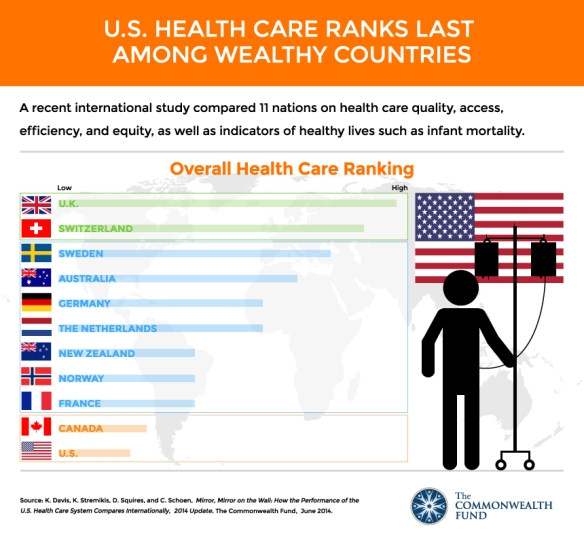
In the long term, I wish for patients and physicians to form a unified platform from which to advocate for policy change. We, patients and physicians, are the end-users of the healthcare system, the largest combined demographic in the system, and I believe we are the ones who benefit the least from the system. Health outcomes for American patients are dismal compared other developed countries, despite our exorbitant expernditures. Physicians kill ourselves at more than twice the rate of the general population.
It’s not enough for medical professional societies to write co-authored, open letters to Congress. It’s not enough for individual patient constituents to stand up at town halls and berate their representatives. We must orient ourselves as resistors in series, rather than in parallel. I think the movement will grow most effectively out of existing connections and relationships, through which we can find shared interests, common goals, and a strong, unified voice for change.
I seek your feedback:
- How do you picture this meeting going?
- How interested are you in learning about physician burnout and how it affects patients?
- If you were invited to such a meeting, what would you think and feel about it?
- What would make you more likely to participate?
- Would you want to host such a meeting in your community? How would you do it?
Thank you for considering, and see you tomorrow!

I think I can respond to #3.
Listening to doctors talk about the pressure they’re under & burnout would scare me & make me even more determined to never seek medical help.
What I need is a better way to talk to my doctor & her clinic. I only get 3 minutes at best to present my issues at an appointment, so I write all my “talking point” down ahead of time. Still, miscommunication happens.
And the clinic is so bound by protocol (I think) that a real, one on one conversation with management is a dream.
I’ve tried writing letters, but I’m usually so angry at that point that I rant, which helps no one.
I hope you have a huge attendance at your group. Let us know what happens.
LikeLike
Hi Sandy Sue,
Thank you so much for your comment, I appreciate that you took the time to write so much. You lay out so many problems with our system today, and I feel badly that this is the reality we live in. I agree, what you (and we all) need is a better way for patients and physicians to communicate–often, effectively, and continuously. I will definitely let you all know if/when this meeting happens! Meanwhile, I’m not sure I can write anything that helps you… but I wonder what patient advocacy groups are actively addressing your concerns on the systems/policy level? It would be great to connect those groups with physician professional societies on these mutually important issues, don’t you think?
LikeLiked by 1 person
This is great! As a physician, I was just asking someone the other day “when did doctors become the enemy?” I think that largely the insurance companies have thrust us into a terrible position with their refusals to pay, micromanagement of care, declining reimbursement leading to ridiculously short appointment times. Plus this “observation versus inpatient” status brought to hospitalization courtesy of Medicare has led to more distrust-even though it’s not a system designed by or even supported by most physicians! I agree that this needs to be changed. We need to go back to being allies! I’m excited about your ideas!
LikeLiked by 1 person
Thank you so much for your comment. So many layers, right? And all completely opaque. It’s a wonder we get anything done at all… 😕
LikeLike
Pingback: 200th Post: The Best of Healing Through Connection | Healing Through Connection
Pingback: How Not to Engage | Healing Through Connection