What’s the most personally fulfilling aspect of your work? In times of uncertainty, threat, and transition, what holds you up?
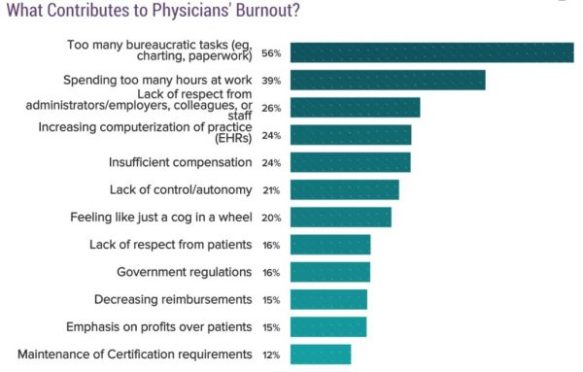
This past week, I had the privilege of standing alongside giants in the fight against physician burnout. In a series of presentations at the annual meeting of the American College of Physicians (ACP), we did our best to acknowledge and validate the current state of physician burnout (about half of all physicians in all specialties report at least one symptom), and then present as many strategies to reduce it as time would allow. We showed how changes in workflow, task distribution, and technology, such as pre-visit labs and scribes, have been shown to improve physician satisfaction, team morale, and patient experience. My role was to attempt to inspire my fellow internists to claim their individual agency, model a culture of wellness, and advocate for systems change in their home institutions.
The content felt dense but manageable, and the audience appeared engaged. Our colleagues from all around the country approached us afterward to clarify studies of efficacy and ask about local representatives for advocacy in the ACP. In the end, I think we achieved our primary objective of having most attendees leave with just a little more hope for our profession than they came in with.
Over the four day conference, however, what consistently grounded me in professional mission and meaning, not only in our own presentation but in others, were the personal stories. That is how we humans relate to one another, after all—through narratives. And connecting to mission and colleagues is key to maintaining a healthy and productive workforce, physician or otherwise.
Our attendees participated in two practices that I’ll share here. Both were “Pair and Share” activities, meant to stimulate reflection both internally and externally.
Who In Your Life Really Changed You?
First we asked our colleagues to think of a patient who changed them, how, and to what end. I know there have been many patients who changed me, but I always think of one particular woman. She was middle aged, obese, diabetic, depressed, and severely disabled from osteoarthritis. She lived alone and had a sparse social network, and her life partner had died unexpectedly a few years before I met her. At every visit we struggled through the same fundamental challenges of weight loss, glucose control, and pain management. How could she take her diabetes medications more regularly? How could we control her pain without having to take opioids every day? How else could we manage her depression, as some of the medications were raising her blood sugar? She may have cried at almost every visit; wailing was not uncommon, and once she even vomited from cumulative distress. Our relationship was good overall. I overcame my impatience with her non-adherence to the treatment plan as I understood her life situation better. But for four of the five years we knew each other, I saw few if any indicators that her thought, emotional, and behavior patterns would change.
Then things started to turn around. She started coming consistently to appointments, no more no-shows. She got online and found a community center that was accessible by bus. She connected with a knitting group and started going to art fairs to sell her creations. She started taking her medications more regularly, and lost enough weight to have her knee replaced. By the time we parted ways, she had transformed from a weeping victim of circumstance to a woman with agency, self-efficacy, and goals, dammit! And most of this had nothing to do with me. I simply had the privilege to witness and support her intrinsic revolution. From her I learned what perseverance looks like; I learned about hope and self-redemption; I learned that I should never make assumptions about anybody’s future.
Who Supported You in a Time of Vulnerability?
They said do the hardest thing that you know you don’t want to do for a living as your first rotation. So I chose surgery. In July of my third year of medical school, my days started around 5:30am and could end the next night at 10pm if my team was busy post call. Most faculty physicians were kind and wise, or at least non-abusive. Some, however, not so much. What buoyed me most through that rotation was always the support and protection of the residents on my team. I would watch them get abused by our attendings, but that sh*t never rolled downhill when the boss left the room. I did not fully realize until years later what a gift that was and how much it spoke to the character of these men (they were all men). This was in the 1990s; verbal abuse of medical students and snide comments about one’s appearance, gender, and just about everything else were simply to be expected. But my favorite residents always pulled me aside and asked how I was. They always made sure I felt confident about my role on the team, and they taught me basic skills with conviction and encouragement. As I was about to insert a patient’s bladder catheter in the operating room, my elder brother in training told me firmly, like he really believed I could do it, “Don’t be afraid, hold it (the penis) like a hose.”
As we did this reflection exercise at the meeting last Wednesday along with our audience, I was so moved by these memories that I looked up one of my old residents that night and sent him a thank you card. I bet he won’t remember at all who I am, but he will hopefully feel validated that he is in exactly the right position now as program director of a surgery residency.
*****
Recalling stories like these, and then sharing them with a person who truly listens, receives them generously, and simply helps you hold them (that was the instruction to the group—when it’s your turn to listen just do that, no interruptions, no jumping in), reconnects us to our calling in medicine. It’s not just about the patients or the science. It’s about all of the relationships and how we tend them.
We will not solve the immensely complex problem of physician burnout overnight. It will take a concerted effort at all levels of healthcare, and physicians cannot and will not do it alone. And it’s not that we are stoic, arrogant, and somehow intrinsically flawed, and thus dissatisfied with our work and leaving the profession in record numbers. It is a systems problem, no question. And, while we call our congressional leaders and professional advocacy groups to change policy, while we lobby our hospital administration to hire more support staff and move the printers closer to where we do our work, we can all take a few minutes each day and reconnect to the core meaning and purpose in that work. Let us all remember a cool story and share it today.