Hey friends, how was your week? Learn anything new and interesting? Anneal any new ideas to existing frameworks in your already complex world view? I did! And it came in another big wave after my presentation on Friday.
I wrote last week about how I put together a new presentation. For the first time, I added the idea of medicine as a complex adaptive system to a talk I gave to physicians at various levels of training and practice. The objective of the presentation was for people to understand the scope of physician burnout, and leave with some ideas of how they could not only cope better themselves today, but also influence the system and move it toward a healthier, more compassionate state in the future.
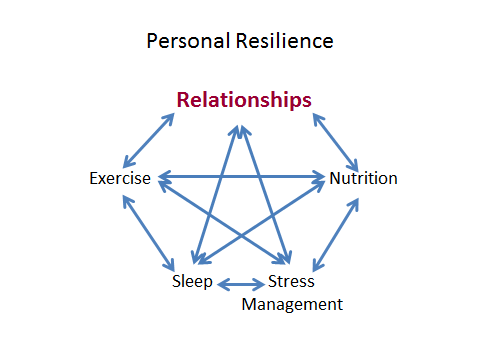
As usual for my talks, I focused first on personal resilience. Many physicians push back at this idea, and rightly so, as many medical organizations have instituted physician wellness programs aimed mainly at ‘fixing’ the doctors with yoga and meditation classes, while allowing the system that burns them out to continue its toxic trends toward over-regulation, loss of physician autonomy, and driving metrics that lie outside of, or even counter to, our core values. I worried that my talk would be taken as just another attempt to tell physicians we aren’t good enough at self-care.
Thankfully, the feedback so far has been positive and I have not heard anyone say they felt berated or shamed. I hope it’s because in addition to tips for self-care (eg 7 minute workout, picnic plate method of eating), I talked about how each of us can actually help change the system. In a complex system, each individual (a ‘node’) is connected to each other individual, directly or indirectly. So, difficult as it may be to see in medicine, everything I do affects all others, and everything each other does affects me. This means I can be a victim and an agent at the same time, and the more I choose one or the other (when I am able to choose), I actively, if unintentionally, contribute to the self-organizing system moving in one direction or another [URL credit for image below pending].

My primary objective in every presentation is to inspire each member of my audience to claim their agency. Before that can happen we must recognize that we have any agency to begin with, then shore up our resources to exercise it (self-care and relationships), and then decide where, when, and how that agency is best directed.
In 5 years of PowerPoint iterations, including and excluding certain concepts, I have always incorporated David Logan’s framework of stages of tribal culture. Basically there are 5 stages, 1-3 being low functioning, and 4-5 high functioning. The tribal mantras for the first three stages are, respectively, “Live sucks,” “My life sucks,” and “I’m great”. Stage four tribes say, “We’re great” and in stage 5 we say, “Life’s great.” The gap between stages 3 and 4 is wide, as evidenced by the traffic jam of people and tribes at the third stage. In my view, the difference is mindset. In the first three stages, most individuals’ implicit focus is on self, and subconscious mindset centers around scarcity and competition. Victims abound in these cultures, as we focus on recognition, advancement, and getting ours. We cross the chasm when we are able to step back and recognize how our mutual connections and how we cultivate them make us better—together—we see the network surrounding and tied to our lone-node-selves.
This week I realized that crossing the stage 3-to-4 chasm relates to two frameworks I learned recently:
The way I see it, in Logan’s tribal culture structure, one initially works toward self-actualization, essentially achieving it when fully inhabiting stage 3, “I’m great.” But crossing to stage 4 requires self-transcendence, as described by Abraham Maslow, by recognizing a greater purpose for one’s existence than simply advancing self-interest. In the same way, through stage 3 we live in what the Arbinger Institute describes as an ‘inward mindset,’ and we cross to stage 4 when we acquire an ‘outward mindset’, which is pretty much what it sounds like. Essentially in stage 3 we mostly say, “I’m great, and I’m surrounded by idiots,” and in stages 4 and 5 the prevailing sentiment resembles, “We’re great, life’s great, and I’m so happy to be here, grateful for the opportunity to contribute.”
An astute colleague pointed out during my talk on Friday that we do not live strictly in one stage or mindset in serial fashion. Depending on circumstances, context, and yes, state of mind and body (hence the importance of self-care!), we move freely and maybe often between stages, sometimes in the very same conversation! The goals are to 1) look for role models to lead us to higher functioning stages more of the time, and 2) model for others around us to climb the tribal culture mountain with us, spending more and more mindset and energy at higher and higher stages.
The problem is the system, and we are the system. So, onward. Progress moves slowly and inevitably. It will take time, energy, and collective effort.
We’ got this.